HS Surgery Guide
Deroofing & Excision
Preparing, recovering, and caring for your wound — a patient-centered guide to discussing surgical options for Hidradenitis Suppurativa with your care team.
Content in this guide is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider regarding your specific medical condition.
Understanding Hidradenitis Suppurativa
HS is a chronic inflammatory skin condition — not a hygiene issue. Understanding it is the first step toward better care.
Hidradenitis Suppurativa (HS) is a chronic inflammatory skin condition affecting the hair follicles. It affects approximately 1–4% of the global population and can occur in anyone, regardless of ethnicity or age.
About 1 in 3 patients report a family history of HS. It is not related to hygiene — it is a systemic inflammatory disease that requires proper medical management.
Surgery for HS focuses on removing diseased tissue to reduce lesions, drainage, scarring, and pain. The right procedure depends on your Hurley Stage and the size and location of affected areas.

Surgical Approaches Your Provider May Consider
HS surgery is not a one-size-fits-all menu. Deroofing and excision are often complementary approaches, and complex HS may require more than one technique depending on tunnels, tissue involvement, location, wound size, closure options, recovery needs, and systemic disease control.
How to Think About the Surgical Decision
Surgery planning should happen with a provider who understands HS. The goal is not to choose the “biggest” procedure or the option with a promised zero-recurrence outcome. The goal is to choose the approach that best addresses the affected tissue, your symptoms, your healing capacity, your responsibilities at home or work, and your overall HS treatment plan.
There is a tunnel, tract, or recurrent draining area that can be opened and allowed to heal from the inside out.
There is broader diseased tissue, complex scarring, or interconnected areas that need more extensive removal.
Some areas need deroofing while others need excision, or when disease patterns vary across body regions.
Time off work, caregiving support, wound size, supply access, and dressing-change support can all influence the surgical plan.
Deroofing
For tunnels and recurring areas
Deroofing is often used for recurring HS areas with tunneling. It can be performed alone or as part of a broader surgical plan. The goal is to reduce pain, drainage, and repeated flaring in a specific area while supporting better quality of life.
Excision
For larger or more complex areas
Considering excision? This video explains when it may be used, what the procedure can involve, and the different ways your body can heal afterward.
Understanding Recurrence in HS
Because HS is a systemic inflammatory disease, recurrence can mean different things. It may mean symptoms return in the same surgical site, or it may mean new HS develops in a different area. New disease elsewhere does not automatically mean the surgery “failed.”
Surgery can reduce pain, drainage, tunneling, and repeated flares in treated tissue, but it does not cure the underlying systemic disease. Biologics and other medical therapies may help control inflammation, but they cannot prevent every future flare or every new lesion for every person.
Your provider should talk with you about what success looks like for your body: less drainage, fewer painful flares, easier wound care, improved mobility, better quality of life, and realistic healing expectations.
A Note on Incision & Drainage (I&D)
- I&D is NOT recommended as a long-term treatment for HS. While it provides short-term pain relief, lesions almost always return.
- There is no evidence that I&D reduces recurrence or promotes true healing.
- If I&D has been suggested for your HS, ask your provider about deroofing or excision as more definitive alternatives.
When Is It More Than a Flare?
HS is not an infection, but it’s important to know when something may be. Understanding your baseline helps you recognize what’s not normal.
- HS is NOT an infection, but antibiotics are sometimes prescribed for their anti-inflammatory effects, not to treat infection.
- Antibiotics may be helpful as short-term or “rescue” therapy, but are not recommended as a long-term solution for HS management.
- A helpful way to monitor changes is to draw a circle around the area and track if redness spreads beyond it.
Spreading redness beyond the usual flare area
Worsening pain outside your normal HS pattern
Fever or feeling unwell — a sign your body is fighting something
Red streaking or stretch mark-like lines extending from the wound
Preparing for Your Procedure
Being well prepared before surgery can meaningfully improve your recovery. Use these checklists to get ready.
Pre-Op Checklist
Home Prep Checklist
Questions to Ask Your Surgeon
Insurance, Work, and Financial Planning
Recovery planning is part of surgical planning. The amount of time you can take off, the help you have at home, and whether supplies are covered may influence the timing, size, and type of procedure your provider recommends.
Before surgery, review:
Ask your employer what paperwork is needed and when it must be submitted. Your surgical team may need time to complete forms.
Check whether your employer offers short-term disability, how much it pays, and whether there is a waiting period.
Larger wounds and secondary intention healing may require more time, more dressing changes, and more support at home.
If someone will help with wound care, ask if they can attend the pre-op visit so they understand supplies, dressing changes, and warning signs.
Insurance Coverage for Wound Care Supplies
Many insurance plans, including Medicaid plans, may cover wound care supplies when they are ordered by your doctor’s office and processed through a durable medical equipment (DME) company. Approval amounts are often based on wound dimensions, drainage level, and how often dressings must be changed.
Ask your provider to document wound size, depth, location, drainage amount, and expected dressing-change frequency. This documentation can make it easier for DME suppliers and insurance plans to approve appropriate quantities.
Recommended Wound Care Supplies
Ask your provider which supplies should be ordered through insurance or a DME company, and keep a small backup supply at home. Some items, like saline and gentle adhesive options, can be hard to find in a hurry.
| Supply | Notes & Tips |
|---|---|
| 4×4 Gauze | Preferred for wound packing and coverage. Stock up generously. |
| Adaptic | Cut to size; prevents gauze from sticking to the wound bed. |
| Kerlix Gauze Roll | Wide-open weave is best; good for wrapping and securing dressings. |
| ABD Pads | Highly absorbent outer layer for larger or smaller wounds. |
| Allevyn Gentle Border | Silicone foam dressings. Gentle and comfortable. |
| Saline Solution | For wound irrigation and moistening gauze. Hard to find — order early. |
| Petroleum Jelly | Safer than Aquaphor for wound beds. Use as a moisture barrier. |
| Hypafix Tape | Preferred tape for securing dressings; gentle on skin. |
| Gloves | Wear gloves for every dressing change to keep the wound clean. |
| Medical Honey | Optional; use only if recommended by your provider. |
| Waterproof Mattress Pad | Helps protect bedding from drainage during recovery. |
| Compression Garments / Mesh Netting | Can help hold dressings in place when tape is difficult or irritating. |
| Front-Zip Surgical Bra or Soft Support Garment | May be helpful for chest, breast, or underarm procedures. |
| Adhesive Alternatives | If you react to tape, ask about silicone-bordered foam, mesh, tubular netting, or clothing-based support. |
Looking for support after surgery? Explore our wound care resources and expert video guidance from Katie Scherling, ARNP.
Recovery and wound care after HS surgery
Healing takes time, consistency, and the right supplies. This section walks through wound healing phases, daily dressing changes, healing expectations, and wound care principles to support recovery.

The Phases of Wound Healing
Understanding how wounds heal helps you set realistic expectations. HS surgical wounds go through three overlapping phases.
Inflammatory Phase
Redness, swelling, warmth, and pain. Your immune system is fighting bacteria and triggering healing.
Proliferative Phase
New tissue fills the wound. Edges begin to contract. New skin forms from wound margins.
Maturation Phase
Scar tissue forms and strengthens. This phase can last up to 2 years depending on wound size and overall health.
Daily Wound Care: Step-by-Step
Follow these steps every time you change your dressing. Consistency and clean technique are the most important factors in healing.
The steps below are general wound care recommendations only. Your surgeon, dermatologist, or wound care team may give you a different wound care regimen based on your specific procedure, wound location, wound size, closure method, drainage level, and healing needs. Always follow the wound care instructions provided by your healthcare team, even if they differ from this guide.
Wash Your Hands & Put On Gloves
Always start with clean hands. Gloves protect both you and the wound from bacteria.
Remove the Old Dressing
Gently peel away the dressing. If gauze is stuck, moisten with saline before removing.
Irrigate the Wound
Rinse the wound with saline solution. Use only what your surgical team recommends. Do not use Hibiclens, hydrogen peroxide, or harsh antiseptics on healing wound tissue unless your provider specifically instructs you to do so.
Apply a Contact Layer
For open wounds, place Adaptic or petroleum-jelly-coated gauze directly against the wound bed.
Apply Filler for Deep Wounds
Lightly fill with saline-moistened gauze to wick drainage and maintain moisture balance. Do not pack tightly.
Cover with an Absorbent Pad
Place an ABD pad or cloud bandage over the contact layer to absorb drainage.
Secure the Dressing
Use Hypafix tape, bordered foam dressing, mesh netting, or clothing to hold the dressing in place.
Dispose & Document
Remove gloves, wash hands again, and consider photographing the wound to track healing.
Wound Care Principles to Live By
These principles guide every successful recovery. Keep them in mind throughout your healing journey.
Maintain moisture balance — not too wet, not too dry.
Do not leave wounds open to air for extended periods.
Do not occlude wounds too tightly.
Do not use Hibiclens, hydrogen peroxide, or strong antiseptics directly on healing wound tissue unless specifically directed by your provider.
Avoid benzoyl peroxide on surgical wounds because it can be drying and irritating to healing tissue.
Neosporin has no proven advantage over plain petroleum jelly and may cause allergic reactions.
Change dressings daily or more often if saturated.
Track your healing with photos to help monitor progress.
Warning Signs — Seek Care Immediately If You Notice:
- Increasing redness, warmth, or swelling around the wound
- Fever over 100.4°F
- Significantly increased pain after the first few days
- Thick, foul-smelling discharge
- Wound edges pulling apart or not beginning to close
- Streaking redness extending from the wound
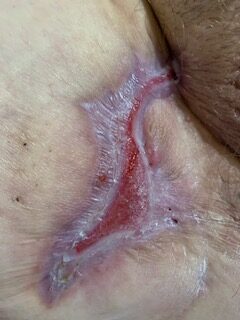
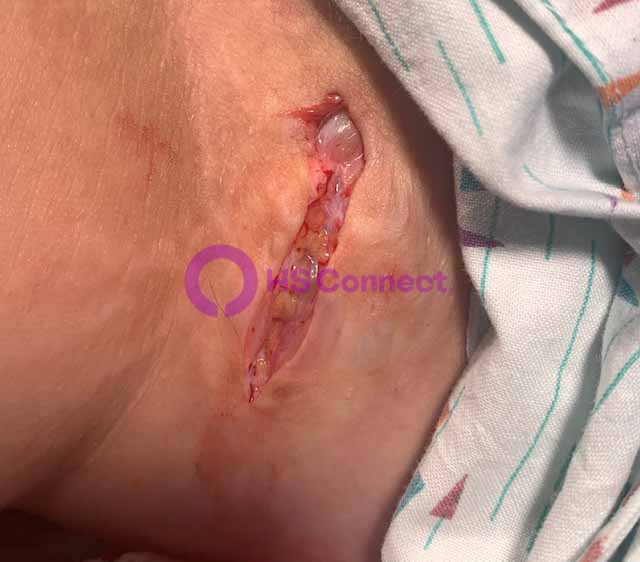
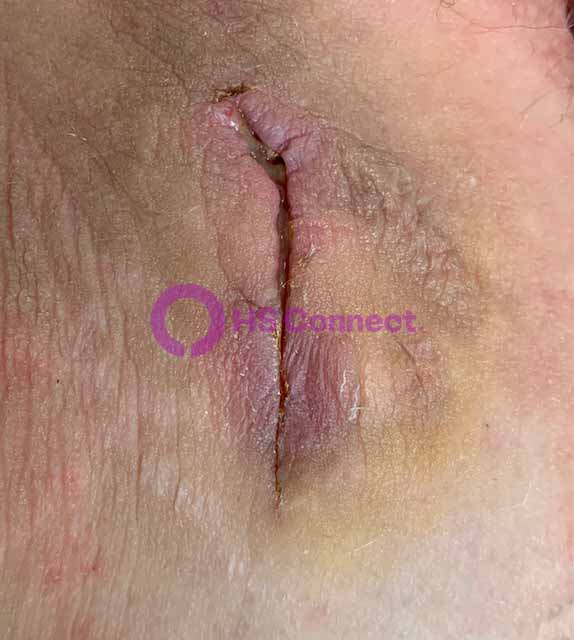
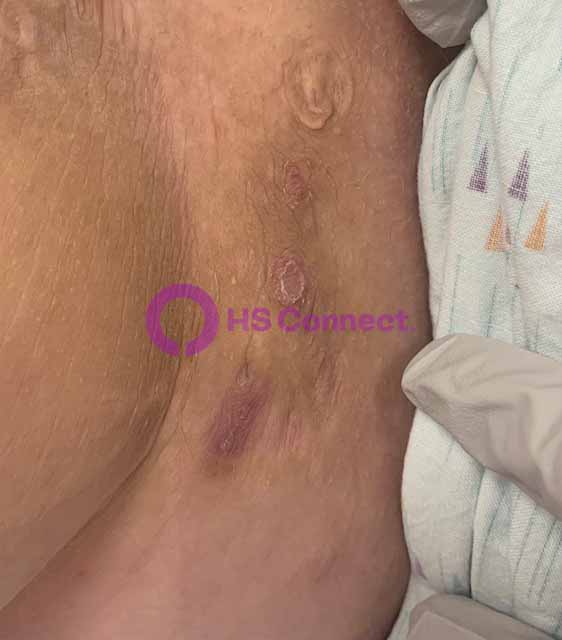
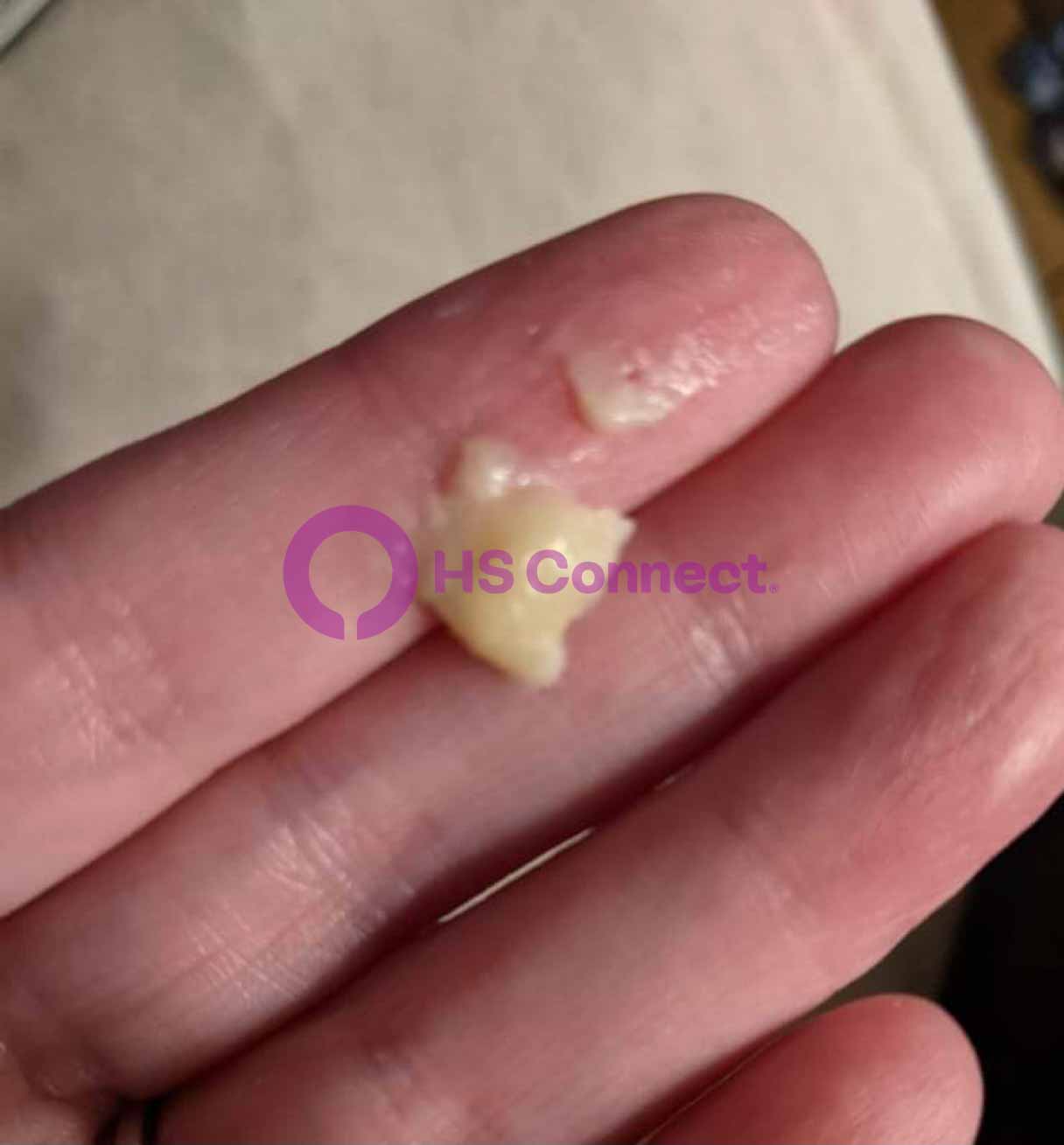
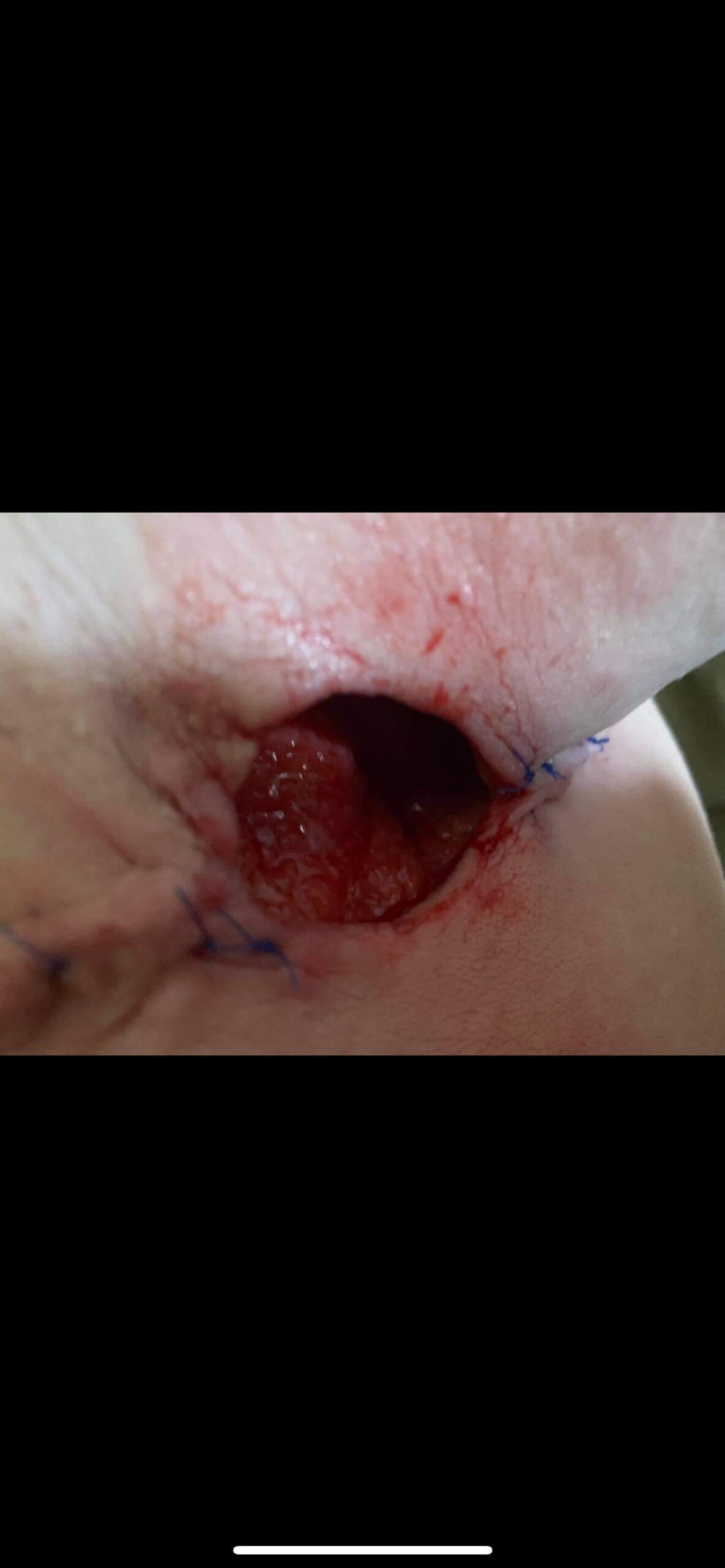
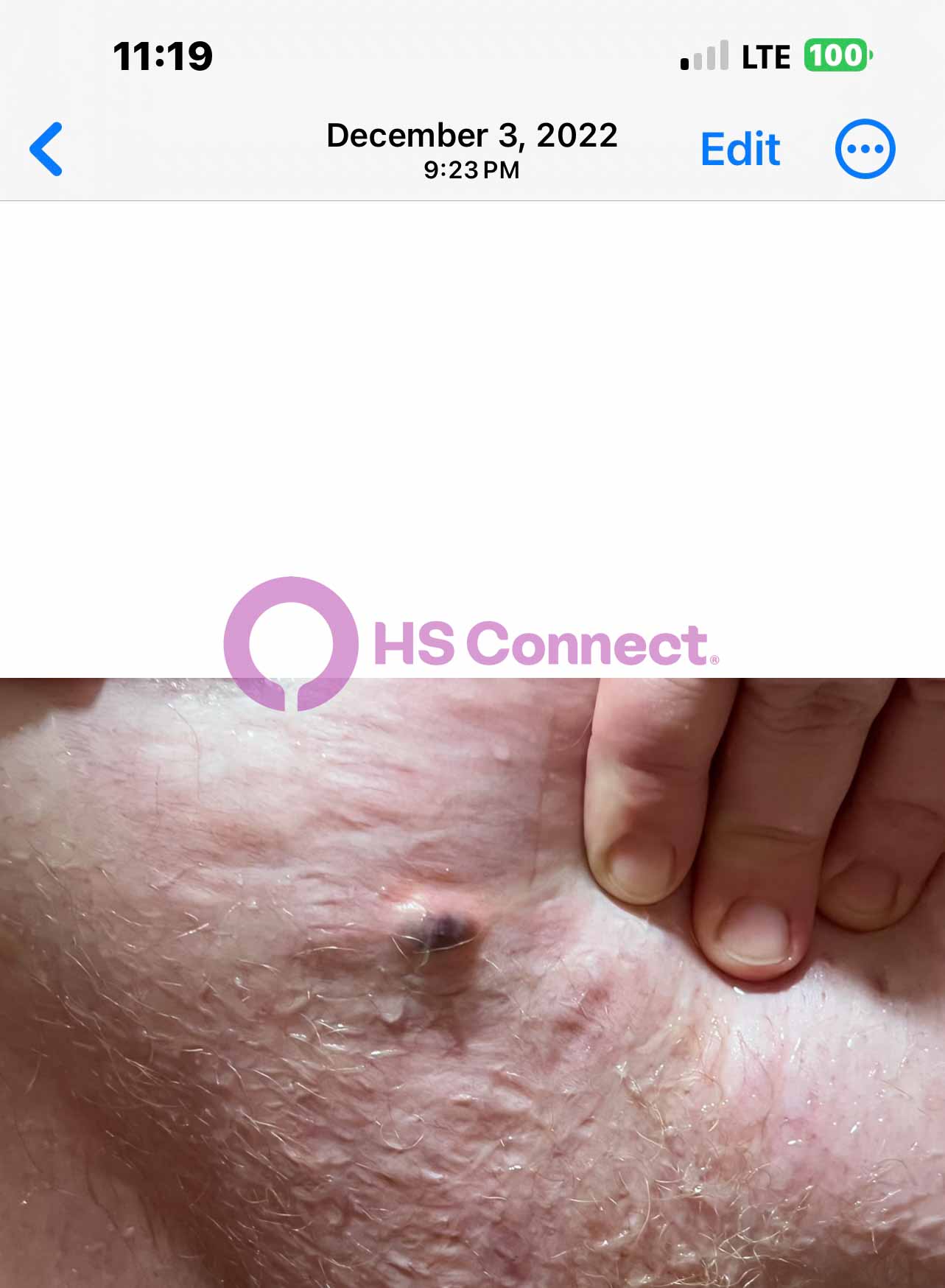
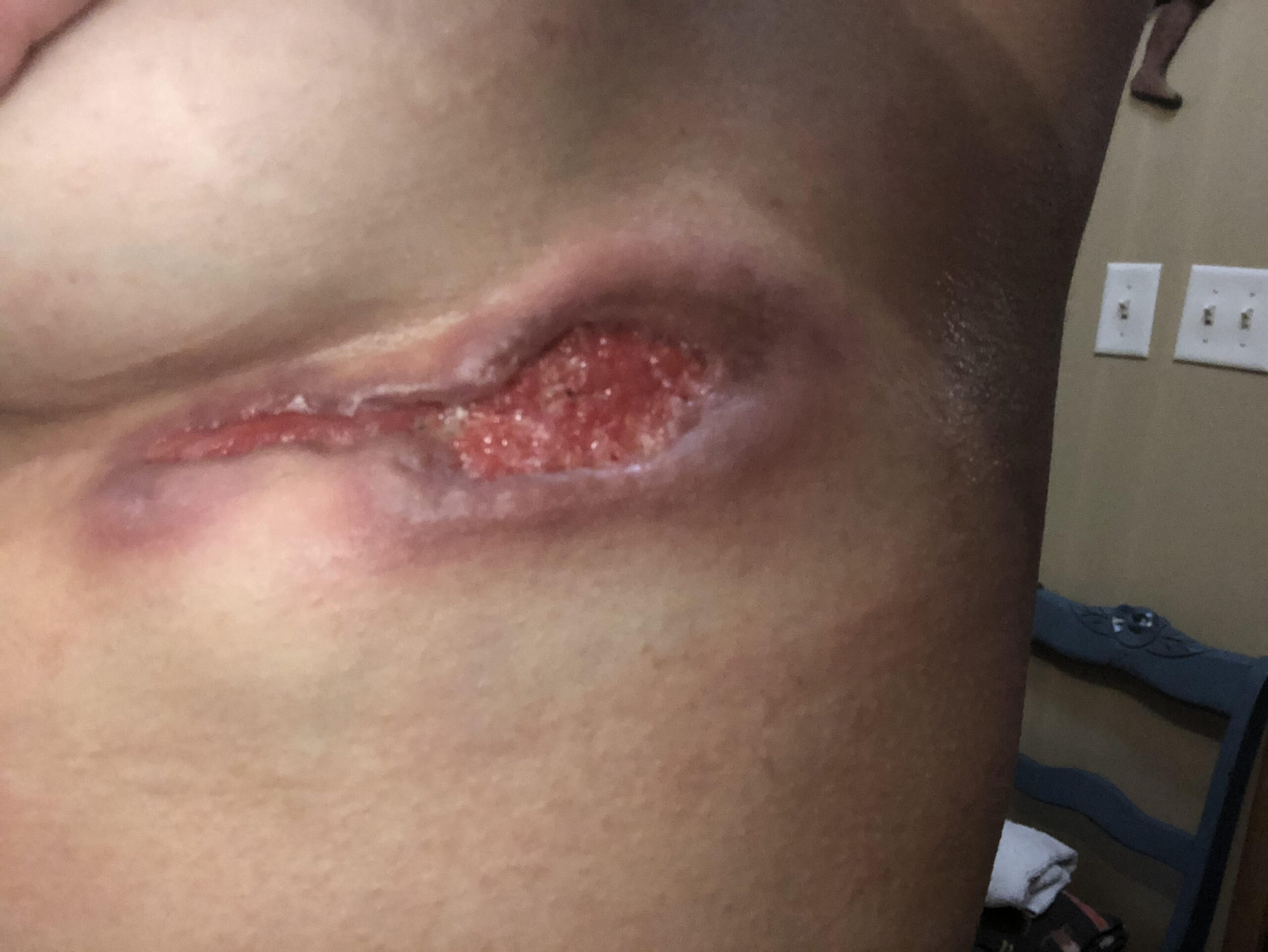
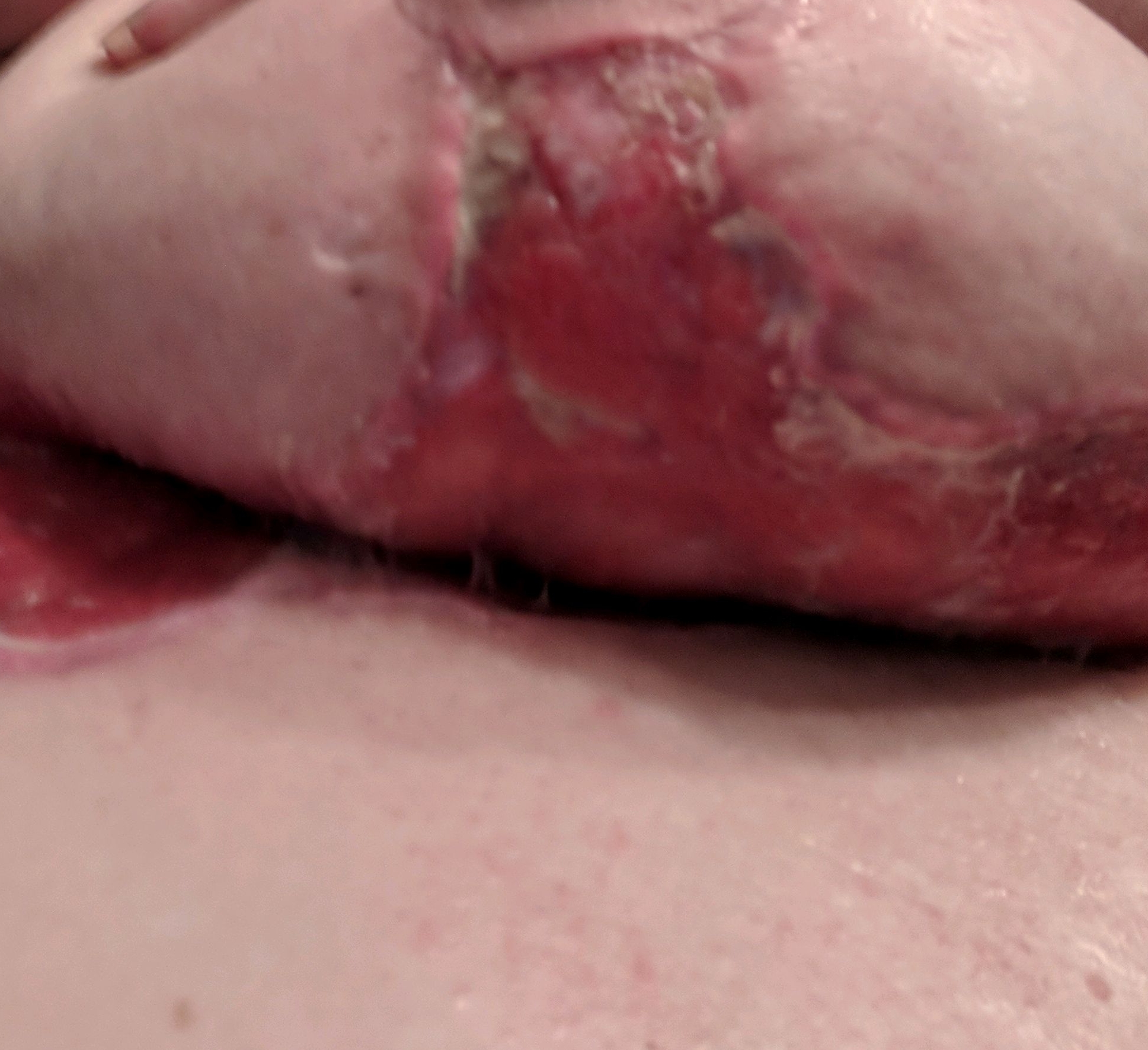
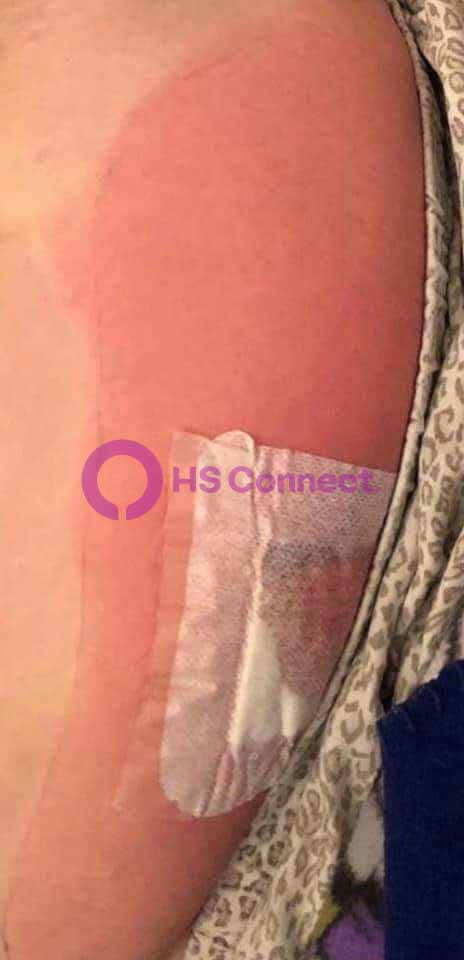
Real photos. Real experiences. Shared to help others understand HS.
These images were shared with consent by people living with HS. They help patients, caregivers, and providers better recognize symptoms, understand healing, and see the many ways HS can appear.
WARNING: Some photos below are graphic in nature and represent real photos of real HS abscesses, surgeries, scars, and healing. All images were shared with consent.